Loma Linda University Health’s milestone highlights the institution’s mission “to make man whole.”

Since becoming the first medical center in the Inland Empire (the greater Los Angeles region) to offer liver transplants to patients in 1993, Loma Linda University Health (LLUH) in Loma Linda, California, United States, has gone on to complete hundreds of procedures — accumulating to 1,000 liver transplants as of March 2021.
“Surpassing 1,000 liver transplants is a huge milestone for the Transplant Institute, carrying out the mission of Loma Linda University to make man whole,” Michael E. de Vera, director of the LLU Transplant Institute, says. “The achievement is more than just a number — it represents the lives of patients touched by the generosity of organ donors and is also a reminder of the countless others on the waitlist who struggle with liver disease and are waiting patiently and desperately for precious, life-saving organs.”

Each year, the Transplant Institute coordinates more than 100 liver transplants performed by surgeons at the LLU Medical Center and enabled by liver donations from deceased individuals who had selflessly agreed to donate.
One of the many liver transplant recipients to benefit from the life-saving procedure offered at LLUH is the 1,001st patient, 56-year-old Albert Richards Jr., who expressed his thankfulness and hopes that sharing his story will inspire some in similar situations to maintain hope and others to enroll as donors.
“I could be here all day talking about the goodness of what I went through,” Richards says, now enjoying his life extension to the fullest and spending time with loved ones who supported him throughout his health journey.
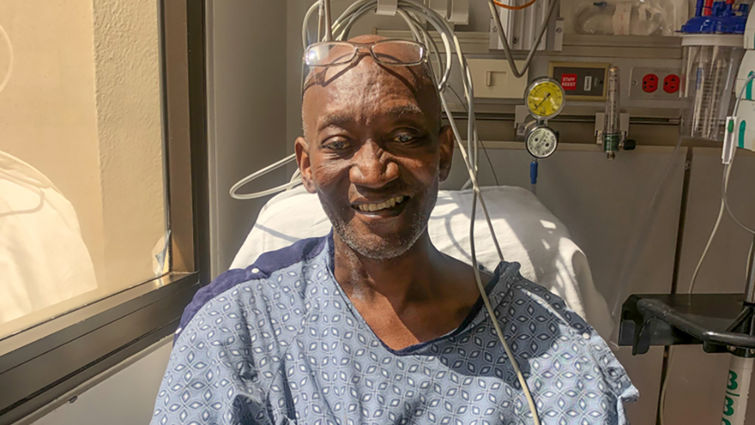
The Las Vegas resident began taking several medications after having suffered from a sudden stroke in December 2016, two of which he discovered years later were not “liver friendly.” Richards started feeling unwell — an unusual circumstance for the 25-year vegetarian, non-smoker, non-drinker, and erstwhile fit owner of a security company.
Blood test results indicated Richards’ liver enzymes were eight times higher than normal. The series of medical appointments that followed confirmed that Richards had a type of end-stage liver disease called non-alcoholic steatohepatitis (NASH) cirrhosis. Nothing was the same after that.
“That was the day that my life changed,” he says. “All of a sudden, the contracts, the invoices, the other duties I had for my business and life … none of that mattered. It was all about health.”
NASH cirrhosis of the liver is the fastest growing indication for liver transplant in the U.S., Minh-Tri Nguyen, the transplant surgeon who performed Richards’ procedure, says. NASH cirrhosis typically occurs in patients with obesity, diabetes, hypertension, and dyslipidemia but may also occur without any of these risk factors, as with Richards. In a subset of patients with fat accumulation in the liver, the liver gets inflamed and subsequently damaged, leading to end-stage liver failure in 20 percent of cases and the need for a new liver via transplant.
Richards joined the liver transplant waitlist in April 2020 and completed video visits with LLUH physicians from both the LLU Las Vegas Hepatology and Liver Transplant Clinic and LLU Transplant Institute to evaluate his health pre-transplant.
“Liver transplant can be a harrowing journey for patients and their families, so we do everything possible to ease their way,” Michael Volk, medical director of the liver transplant program at the Transplant Institute, says. “We are proud to be the transplant center for all patients in the Inland Empire and southern Nevada, for whom it’s easier to get to us than anywhere else.”
Nguyen says that patients on the waitlist for a new liver are prioritized by their Model for End-Stage Liver Disease (MELD) score. A MELD score above 30 predicts a 90-day mortality greater than 50 percent. MELD scores range from 6 to 40 and are based on a calculation of four factors: (1) bilirubin: how effectively the liver excretes bile; (2) INR or prothrombin: how well the liver can produce blood clotting factors; (3) creatinine: the current function of the kidney; (4) sodium: an electrolyte that is a marker for significant liver disease.

Richards’ MELD score fluctuated around the mid-20s to low 30s. He experienced complications such as ascites — fluid buildup inside his abdomen that causes bloating — and hepatic encephalopathy that occurs when the liver cannot effectively clear out toxins from the bloodstream, thus affecting the brain and leading to fatigue, confusion, and even coma in severe cases.
The long-awaited call announcing that a liver was available for Richards came in mid-March 2021. Upon his arrival at LLUH, however, physicians determined that this particular liver was too large for his abdomen. He waited a week for another liver to become available, during which his MELD score spiked to 36. Despite the ups and downs, Richards says, his family and LLUH care team worked tirelessly to ensure his well-being as he awaited a transplant.
“Words are not adequate to describe how God blessed me and how the doctors and nurses were so supportive,” Richards says. “They really got me through it. They gave me all the information that was needed, visited me throughout the day, and kept me in the loop with everything — from medications to different tests.”
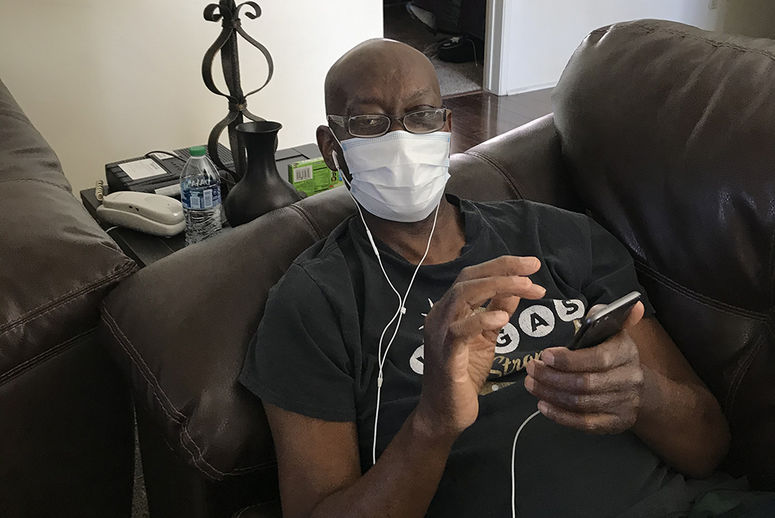
Soon enough, another liver became available for Richards. On Friday, March 19, 2021, he awoke post-procedure and instantly felt the improvement in his physical and mental health. He says he looks forward to spending precious time with his mother, three siblings, a daughter, and two grandchildren. He plans to write a memoir of his life and recent experience for his grandchildren, typing on his laptop that has a sticky note stuck to it: “No bad days,” because, he says, every day being alive is a good one.
“I thank God for the wonderful donor and their loved ones who have granted me another opportunity to do something even greater in life and continue striving to be an outstanding person,” Richards says. “Every opportunity I get to share what I’ve gone through with others, I want to be able to do that.”
Not long ago, Richards was one of the more than 11,000 people in the country waiting for a liver as a lifeline. Nguyen says the milestone of 1,000 liver transplants at LLUH is one worth commemorating. Yet, the work is never done for the LLU Transplant Institute, as the only liver transplant program in the Inland Empire and second-largest deceased donor liver transplant center in Southern California. There are always more lives to save.
“Over the decades, our transplant program has grown significantly and allowed us to serve many patients from the Inland Empire and beyond,” Nguyen says. “We are looking forward to treating the next 1,000 patients, starting with Mr. Richards.”
The original version of this story was posted on the Loma Linda University Health news site.








